The Achilles tendon gets its name from Greek mythology.
A famous warrior, Achilles was vulnerable only in the narrow part behind the ankle where his mother grasped the baby when she dipped him in the River Styx, to shield him from mortal harm.
The tiny ankle not coated in magic water was his undoing, as an arrow from his enemy caught him in the Achilles tendon and led to his death.
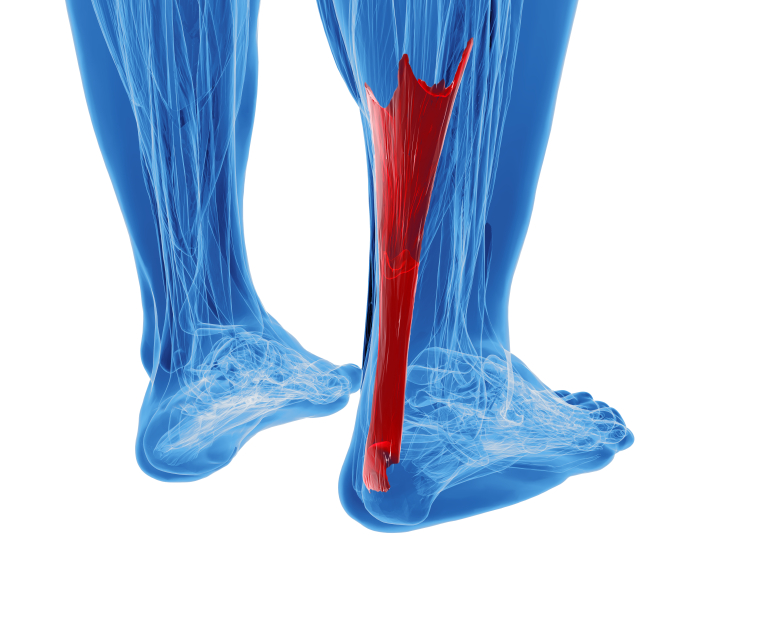
Mythology aside, the Achilles tendon is a site of modern injuries, common but treatable. The Achilles is the longest tendon in the body, running down the back of the leg from the calf muscle to the heel bone. It enables us to lift the heel off the ground so we can walk.
Achilles tendinitis is an inflammation of this ligament that can be caused by overuse or trauma. The condition can come on gradually or with a loud ‘pop’ that sounds ominous. If left untreated, Achilles tendinitis can lead to the development of bone spurs or a ruptured tendon.
Certain kinds of movement can cause sudden damage to the Achilles. Think of a tennis player rushing the net and then pedaling backward to hit an overhead smash.
More often, we see Achilles tendinitis in people who spend long hours on their feet, such as teachers or waitresses.
Then there are the weekend warriors who fight their battles only once weekly, while the rest of their days are spent sitting in automobiles or in cubicles.
A sudden increase in training or an abrupt change in technique can also trigger inflammation of the Achilles tendon.
Treating an Inflamed Achilles Tendinitis
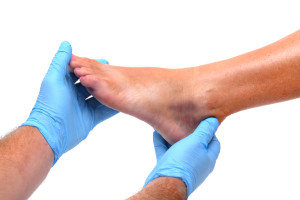
Before we can design a treatment plan, we first must determine the nature and severity of the injury.
There are two general types of Achilles tendinitis: non-insertional and insertional.
These terms refer to whether the inflammation is concentrated in the place where the muscle inserts into the bone, or whether it is located in the fibers in the middle part of the tendon.
While x-rays help the doctor see whether the lower part of the tendon has calcified (indicating insertional tendinitis), an MRI is useful in cases where surgery is being considered.
While most cases of Achilles tendinitis can be treated with nonsurgical therapy, Achilles tendinitis is notoriously slow to heal. If you had pain for several months before calling the clinic, it could take up to six months for the treatment to take effect.
Our first recommendation is to stop the activity that’s causing or exacerbating the pain. If you are a runner or you engage in some high-impact sport such as tennis or soccer, switch to a different activity that places less stress on the tendon. Biking and swimming are possible cross-training alternatives.
Prognosis Depends on Patience
Nonsurgical options rely on reducing the irritation that caused the inflammation in the first place. Icing the injured leg can help. Anti-inflammatory drugs are sometimes advised. There are exercises that help strengthen the calf muscles and relieve stress on the tendon, but one must be careful because some exercises can actually worsen the strain on the Achilles. Check with your doctor or physical therapist before launching any Achilles-related exercise therapy.
Cortisone injections are seldom recommended because they have been known to cause the tendon to rupture.
Insertional Achilles tendinitis can be alleviated by wearing a specific type of heel, or heel lifts. For patients with a great deal of pain, a special boot is sometimes prescribed. Long-term use of the boot is not recommended, because it can actually weaken the calf muscle.
If the tendinitis hasn’t responded after six months of conservative treatment, we may discuss orthopedic surgery. While most patients are able to return to the activity or sport they love after Achilles tendinitis, there is a small chance that you will not have that option— still another reason to investigate cross-training.