This oldest of sports injuries is now thought to involve damage to non-rejuvenating tissue. So it’s best to take care of what we are born with.
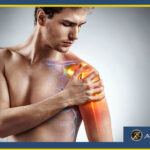
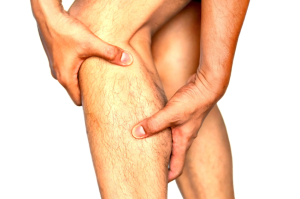 It’s one of the most common injuries in sports medicine, the Achilles tendon rupture, or tear. This tendon, largest in our body, is formed from the medial and lateral heads of the gastrocnemius and the soleus. The first two originate above the knee and the third originates below the knee.
It’s one of the most common injuries in sports medicine, the Achilles tendon rupture, or tear. This tendon, largest in our body, is formed from the medial and lateral heads of the gastrocnemius and the soleus. The first two originate above the knee and the third originates below the knee.
The Achilles tendon has some unusual features. One, it’s not covered by a sheath like other tendons; instead it’s surrounded by a layer of fatty tissue that supplies blood, called the paratenon. Another thing that’s different is that the fibers in this tendon seem to be permanent, like our teeth. They don’t regenerate like other muscle fibers. What does this mean to you, Sportsperson?
It means we need to take care of our Achilles, not treat it as a throwaway.
Early intervention is best. If you start to feel an ache in the back of your leg between the foot and knee, it may be a signal to change your training regimen. Same goes if you notice swelling. This is an injury that can’t heal unless it has some down time. Make an appointment to have it examined before it becomes a chronic condition, which is more difficult to resolve.
Main Cause of Tendonitis: Overuse, Fatigue
Just about anyone who trains hard or competes has some risk of straining or tearing this tendon. But there are factors that predispose a person to Achilles tendonitis (or tendinitis, as it’s sometimes spelled):
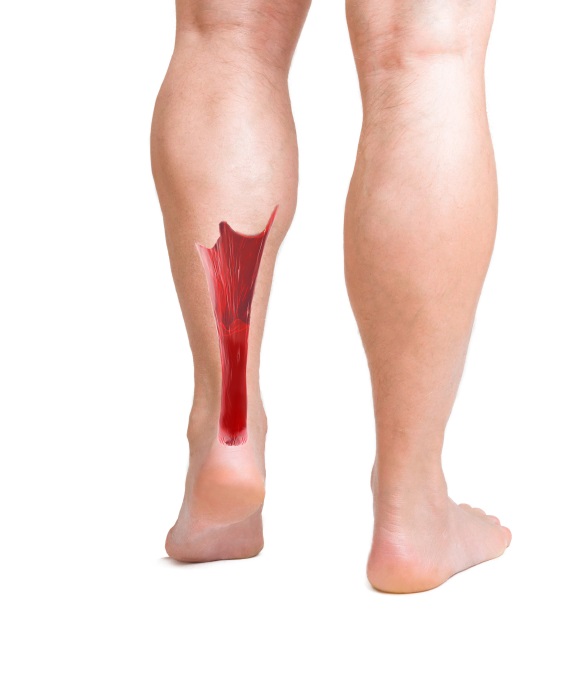
- A tired Achilles is vulnerable.
- Inflexibility: Stretch early and often, but not so hard that you feel the tendon tightening. Tendons aren’t designed to be over-extended, and can be damaged by excessive stretching.
- Sudden changes in training methods, terrain, equipment or intensity can cause a sudden injury.
- Any of a class of antibiotics that includes Cipro (the FDA is looking into this) makes a person vulnerable to Achilles tendonitis.
- Ditto for the prior use of oral steroids.
We usually treat a mild strain conservatively, at first. Therapy might include a cast, boot or splint to restrict movement, and possibly physical therapy. We can ascertain the nature and severity of the injury when we examine you. One rule of thumb is that the tendon is involved if the painful area seems to move when you grasp the injured calf and flex your ankle and foot. If the painful area is stationary, it could be the paratenon instead of the tendon. As for the exact nature of the strain or tear, a thorough physical exam is necessary.
When Is Surgery Called For?
Some say that Americans are too quick to recommend surgery, and that other nations allow their Achilles problems to heal in due time. The problem with this approach is that athletes are not always patient. (They may be patients but they’re not always patient.) If you are an athlete and time is critical, surgery might be the best option.
Another issue is longterm recovery. Studies suggest that patients who are treated surgically have a more complete recovery and less risk of re-injurying the Achilles tendon than those treated conservatively.
One study by researchers in Halifax, Nova Scotia, showed that nonsurgical treatment was as effective as surgery, but only if it was accompanied by a strict program of functional rehab.
As for prevention, cross-training is always preferred. An athlete who spends all of his or her time repeating the same motion is asking for trouble. And even when cross-training, moderation is the word. The old 10% rule (increasing the duration of any workout by a maximum of 10% each week) might be too gradual for many of us but certainly we should be wary of abruptly jumping to another level, either in terms of time or intensity.